IUI and ICI
Definition
Intrauterine Insemination (IUI): A type of fertility treatment that involves placing washed sperm inside a woman’s uterus close to the fallopian tubes in aim to increase the chances of conceiving.
Intracervical insemination (ICI)– Unwashed or raw sperm is placed in the cervix. This procedure can be done at home and is sometimes called intravaginal (IVI) insemination
History of IUI
Intrauterine Insemination first originated back in the 14th century by the Arabians it wasn’t created for the human reproduction purpose though it was to breed their stallions. In 1742, fish eggs were successfully fertilized by Dutch scientists. Then in 1784 Lazarro Spallanzani an Italian catholic Priest/Biologist/Physiologist started using this technique for Dog breeding.
Although some resources out there claim that in the 1400s that King Henry IV of Castile unsuccessfully attempted to artificially inseminate his wife. The first successful recording of human conception via this method happened in London in 1793 and was accredited to John Hunter a Scottish Surgeon.
Hunter put his surgical skills to use by working with a patient who had hypospadias which is the inability to ejaculate sperm. Making an incision into this husband’s testes he was able to extract the semen and insert the sperm into that man’s wife’s cervix similar to the turkey baster method.

In 1866, a controversial American physician dubbed “the father of modern gynecology” James Marion Sims attempted IUI with six women. Although he experienced low success rates because he didn’t understand a woman’s fertile window and mistook menstruation as the ovulation period.
In 1899 Ilya Ivanovich Ivanov a Russian and Soviet Biologist who specialized in the field of artificial insemination and the interspecific hybridization of animals. He was a pioneer is studying Ai for domestic farm animals, dogs, foxes, rabbits, horses, and poultry. He developed Semen extenders and came up with the idea of using superior stallion sperm to pass on those genetics to breed higher quality stallions.
From there many researchers all across the globe started doing their own research and expanding on artificial insemination in the 1930s Cattle artificial insemination using frozen sperm exploded in the USA. Soon to follow was cryopreservation for humans that facilitated sperm preservation for later use, using IUI techniques.
The IUI procedure back then were most suited for couples with male fertility problems, such as impotence or vaginismus or those who experienced hostile female cervical mucus thats annilahates any sperm that comes into it’s path.
In 1997 in Milan (Italy) the concept of Washing sperm was invented. The thought behind it was to allow men who were infected with HIV to have children without infecting the mother or child. (Also discussed in Episode 31 of the podcast). IUI before such times was previously done without washing sperm technique, the thought of incorporating extra protection against STDs and that a small minority of women who experienced semen allergies caused by the prostaglandins present in the semen that could cause mild to severe cramps was something that quickly became standard procedure throughout the world. In saying that though on the IVF Australia website “An IUI procedure is performed by a nurse and is usually not painful, although sometimes you might feel mild cramping and/or discomfort. You should be able to return to work straight away.” Regardless of Semen being washed or not it appears to be considered the norm.

In modern times with the fertility business booming and the rise of the sperm donor industry, IUI is used as a stepping stone before more invasive procedures such as In Vitro Fertilization (IVF.) Most clinics in their business model will try to entice their customers into trying IUI before moving you on to the more realistic chance of conceiving via IVF.
So is IUI worth the cost it in a clinical sense?
Recently, as people become more educated the popularity of IUI has decreased substantially with the introduction of newer and more successful techniques such as IVF and DIY home insemination having a greater chance of achieving pregnancy. However, IUI remains a viable and lower-cost option for recipients seeking pregnancy that haven’t done their homework online about the world of online sperm donation with fresh and higher motile sperm.
| Woman’s age | Pregnancy rates | Delivery rates |
| 20-30 years | 17.6% | 13% |
| 31- 35 years | 13.4% | 10% |
| 36-38 years | 13.3% | 9% |
| 39-40 years | 10.6% | 7% |
| 40+ years | 5.4% | 3% |
There is a lot of conflicting data out there about IUI success rates with a lot of people in the industry just rounding it up to about a 20% chance. For a person under 30 that is a 1 in 5 months of trying at a clinic based on the law of averages. Then why do the clinics usually only recommend a couple of cycles of IUI then before moving you onto IVF? It’s all about their business model get you paying for a couple of low chance options before getting you started on IVF money in the bank for very little work on their behalf.
Explanation as to why IUI Success rates are low
The amount of Sperm given in the Insemination
So why are IUI success rates so low compared to at-home Artificial Insemination. First of all, most clinics will only give 0.5mls of sperm (in a vial or often referred to as a straw), a sperm donor via our Sperm Donation World communities will give you roughly 2 to 10ml which is potentially 4-20 times more than the amount you’re getting from the clinic in single dosage, and a donor may also give you more than 1 donation per cycle as well to increase chances of conception that cycle. Potentially what a Donor may give you in 1 cycle of trying could be divided up to over a year’s supply of trying at a clinic.
If you thought 0.5mls provided was a low amount already well hold on a just one second, it gets better you can’t just put sperm in the freezer it has to be mixed with a cryoprotectant if you’re not familiar with the term it is a substance used to protect the sperm from freezing damage. So essentially the straw contains 0.25mls of sperm and 0.25mls of the freezing agent.
The Washing Process
The Sperm is “WASHED” a term they use to try and upsell It to you that It is clean and that it is good this way. There are several problems with this procedure, it’s not like putting your dirty plates into a dishwasher and clicking the go button, it’s quite a technical process, there is a set precise way that it must be done. If a technician isn’t trained properly or doesn’t care, or pays a lack of attention to detail, the sperm can die very easily when done wrong, there have been studies done where sperm count tests are done prior to and after the wash process, and the numbers have come back at abysmal levels. If you go down this path you need to watch videos online and ask your clinic what training the technician has in the art of washing sperm.
The Freezing Process
The Sperm has been washed and the ones that have survived that part, now have to be frozen and later have to survive the freezing process. The Freezing process is brutal only 50% of the sperm will survive and the ones that do make it take a drastic reduction in motility often losing 20% rates. It is believed that if the freezing process is strong enough to kill half the sperm, what long-term impact does it have on the sperm that survive as it considered they must have taken some DNA damage to the cells and will the child conceived from this process overall lifespan be compromised?
Booking the Appointment and the timing of the insemination
When you’re using frozen sperm your window is shortened as the lifespan and the strength of the sperm are weakened so the timing of your insemination is essential ideally the egg needs to be released within 12 hours although can last up to 24 hours. As opposed to a fresh donation that is more likely to be functional up to 24 hours to 48 hours.
Most clinics make your book your appointment in advance that may not always align with your peak timing jeopardizing the chances of conception. Also, some clinics are not weekend friendly so if your peak does is on Sunday that doesn’t help either. They may try and trigger shot you at a cost to bring it forward.
Most clinics will only give you one insemination per cycle rather than stagger them over a couple of days to cover your window.
How can you Improve the IUI Success rate
If you elect to go down the IUI path then you need to do everything in your power to help increase the odds from factors that you can control. Creating a healthy environment for pregnancy is essential for IUI success. Somethings to consider are.
- If you’re a fitness fanatic reduce your exercise regimen keeping things simple and low impact
- Support a healthy pregnancy by taking prenatal vitamins (check out here for the recommended vitamins)
- Eating well and consuming a healthy diet will promote overall health after IUI for success
- Stay hydrated and toxin-free by drinking lots of water
- Find ways to reduce stress (a lot of evidence shows stress can reduce your chances of getting pregnant)
- Ensure to put legs up and stay put after insemination for at least 15 minutes. A Netherlands study found it to increase success rates

Can you do IUI at home?
Some women are allergic to Semen because of a certain protein found in it Gynaecologists can test if you’re allergic, however while not rare it’s not particularly common, which leads me to the question are clinics simply washing sperm to protect the minority who may have allergic reactions?
In my time I have come across several women within the Sperm Donation Australia community that had Dr. Robin Munro as their Gynaecologist/Obstetrician located in Bendigo, in Victoria. He is now retired as he must be over 70 years of age. Women from within my group were offered after clinical hour times for $100 an IUI service, that their donor could drop off fresh sperm and Dr. Munro would inseminate the whole lot via IUI and unwashed. All they said was they had to show Dr. Munro a donor contract and he was satisfied to perform the procedure.
Of the women, I spoke to they had done their fertility tests done previously, so I am sure Dr. Munro would have known they were not allergic to semen, and none reported that they had any ill effects from unwashed IUI. One of these women had been trying for 2.5 years with various methods, the first time she tried unwashed fresh IUI with the full amount of donor’s sperm she was pregnant!
Witnessing such stories like Dr. Munro’s procedures and the countless do-it-yourself inseminations at home that community members have taken upon themselves to perform at home IUI, I am still caught in two minds about the seriousness of washed/unwashed sperm. The fertility clinics have always used tactics of manipulation and controlling people via fear in order to keep people in their systems and prior to 1997 IUI was done with unwashed sperm.
The whole thought process on why some people elect to choose to do at home IUI is it eliminates contact with the vagina’s acidity conditions, it then bypasses the cervical mucus in the cervix, while that is considered a more sperm-friendly environment than the vagina’s acid a lot of sperm get trapped and stuck to the sticky cervical mucus stopping them from entering the uterus.
It comes as no surprise by bypassing these elements that Home IUI has had reported higher success rates than clinical IUI as you’re using more lively fresh sperm, you’re also receiving more sperm as the donations haven’t been divided up and you may also be doing a couple of inseminations per cycle.
Although we have seen considerable higher success due to rogue IUI it’s not something I can endorse just in case someone did have an adverse reaction, so it’s something you consider based on your research and dialect with a professional.
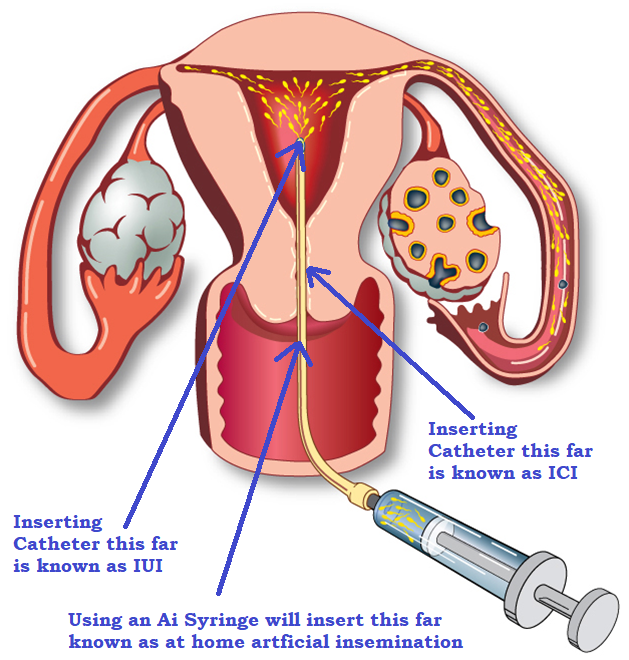
Can you do ICI at home?
Intracervical insemination (ICI) is one of the oldest and most common artificial insemination procedures, dating back as far as the 1880s. Similar to intrauterine insemination (IUI), it involves placing sperm directly into the woman’s reproductive tract to improve the chances of pregnancy.
So are you able to do this at home? the short answer is yes you can! but do your research! Using a speculum and catheter that you can buy in an ICI/IUI Kit here will help the process.
The point of ICI is to bypass the Vaginas acidity conditions altogether and also to bypass a pit of the cervix. The average Cervix is 3 to 4 cm. So to insert the catheter in a couple of centimetres into the cervix still allows the cervix to filter out the semen but giving the sperm less further to travel into the uterus.

If you want to take extra precaution you could ask for an ultrasound to see just how long your cervix is to make sure you’re not inserting the catheter in too far otherwise it turns into IUI that comes with the higher risks previously mentioned.
Summary
Social Media Trying to Conceive groups can create a delusional reality without breaking down the numbers, it can be confusing. For example; So you’re looking into IUI and you post a question. Let’s say you joined a IUI group with 10,000 members and you want to find some comfort in IUI works so you do a post asking who has been successful. Now out of those 10,000 that done IUI roughly 1500 of them are going to have a first-time success (15%). Normally everyone who had early success love screaming from the rooftops they love sharing their triumphant success especially when it comes to their little baby. Reading information like this from multiple people makes it’s very believable in our own minds that achieving the same result is a realistic possibility. The reality is of those 1500 there is 8500 that didn’t get this result but people are less likely to talk about an issue that saddens them.
Unless you have PCOS and taking gonadotrophins during your cycle, it’s In my honest opinion IUI in a clinic setting to put it bluntly is a waste of time and money for anyone over the age of 27, if you want to do a less invasive procedure than IVF then at home artificial insemination is your more realistic option for a conception. If you’re wanting to go to a clinic for whatever reason skip the small talk go straight to IVF.
Purchase a IUI/ICI Kit
ICI/IUI Insemination Kit
The Grand Daddy Deluxe Artificial insemination kit
Related Sources:
IUI Success Rates
